Bipolar Disorder and ADHD Treatment Center

Bipolar disorder and ADHD have similar symptoms. And because these symptoms look so much like a presentation of either bipolar disorder or ADHD, they’re often misdiagnosed.
What Is ADHD and Bipolar Disorder?
ADHD is characterized by persistent patterns of inattention, hyperactivity, and impulsivity, often noticeable in childhood and affecting daily functioning. Bipolar Disorder involves extreme mood swings, including episodes of mania (elevated mood, increased activity) and depression (low mood, low energy). While ADHD primarily affects attention and behavior, Bipolar Disorder impacts mood regulation. Both conditions require proper diagnosis and treatment, often involving medication, therapy, and lifestyle changes to manage symptoms effectively.

Comorbidity of Bipolar Disorder and ADHD
Bipolar disorder, a mood disorder, and ADHD, a neurodevelopmental disorder, are commonly recognized as conditions with a high degree of comorbidity. That means they often co-occur. There’s a biological link between the two conditions.
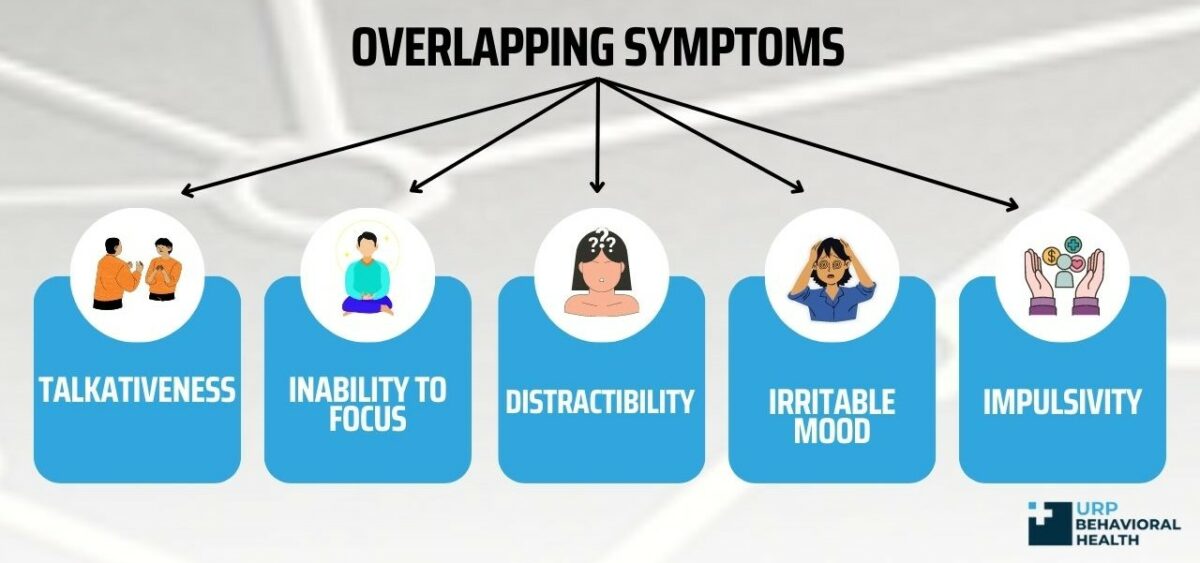
Other Symptoms of Co-occurring Bipolar Disorder and ADHD
When develop co-occurring bipolar disorder and ADHD, you experience manic episodes as part of bipolar disorder. It includes symptoms like elevated mood and an inflated sense of self. Also exhibit symptoms of a major depressive episode, such as low mood, lack of interest in activities you previously enjoyed, fatigue, feelings of hopelessness, and thoughts of death.
With ADHD, show symptoms of inattention, hyperactivity-impulsivity, or both. Inattention is characterized by failing to notice important details, poor ability to organize tasks, and forgetfulness. Meanwhile, hyperactivity can include symptoms like fidgeting, poor planning and execution, and feelings of restlessness.
Treatment For Bipolar Disorder and ADHD
At URP Behavioral Health, we specialize in accurate diagnosis and personalized treatment plans for individuals with ADHD, Bipolar Disorder, and co-occurring conditions. Our goal is to improve quality of life through comprehensive care tailored to each person’s unique needs and challenges. Mental health practitioners carefully implement aspects of treatments for both conditions.

Treating Bipolar Disorder
For bipolar disorder, treatment involves a combination of medication, psychotherapy, and wellness therapies commonly known as holistic treatment.
Medication prescribed for manic episodes includes mood stabilizers, which can help prevent mood imbalances. In cases of severe mania that leads to psychotic features, antipsychotics are prescribed as well.

Treating ADHD
Once manic symptoms have been managed, practitioners may prescribe medication to address ADHD symptoms. Because medication includes both stimulant and non-stimulant formulations, practitioners should prescribe whichever drug is best for current circumstances.
Since stimulant medications can potentially trigger a manic episode, the type of drug and dosage should be considered on a case-by-case basis. Moreover, psychotherapy can help address certain ADHD symptoms by teaching the client new skills that help with maintaining concentration, emotional regulation, and more.

Improving Wellness
In addition to taking medication and attending therapy sessions, making meaningful changes to your lifestyle can have a big impact. This includes getting regular exercise, eating a balanced diet comprising whole foods, and setting a specific sleep schedule. Additionally, engaging in holistic therapies like meditation, animal-assisted therapy, and therapeutic massage can help alleviate stress, which is a common trigger for symptoms.
Where Can People Go If They Have Bipolar Disorder and ADHD?
Getting a diagnosis of ADHD or bipolar disorder can take time. And if you present with symptoms of both conditions, it can take even longer to get an accurate diagnosis. Due to the overlapping symptoms and similarities between the disorders, your mental health practitioner will need to perform an extensive evaluation.
At URP Behavioral Health rehab center, diagnosing ADHD bipolar disorder and involves comprehensive evaluations, differential diagnosis, and behavioral testing. We use personalized approaches, combining expert medical assessment with modern techniques to ensure accurate diagnosis and effective treatment plans.
ADHD Vs. Bipolar Disorder in Adults
The major difference is that symptoms of ADHD are situational and contextual, but in bipolar disorder, your symptoms don’t occur as the result of external factors. When people with ADHD are in a positive and stimulating environment, they can maintain a better mood. And when the environment fails to provide adequate stimulation, they can end up feeling agitated and bored. People with ADHD will see the world around them in the same manner, even as their mood changes. Similarly, they can control their feelings by changing the environment and stimuli around them.
Bipolar depressive episode occurs as a result of an internal emotional state. It’s not triggered by situational reasons – you just wake up and feel different when you’re depressed versus when you’re not.
Treatment In Case Of Unclear Diagnosis
When it’s unclear whether the has bipolar disorder, ADHD, or both, clinicians prefer to start with ADHD treatment. Many people get diagnosed with ADHD around the age of 12.
The average age of diagnosis in bipolar disorder is 25. That’s because it often develops after adolescence. So, even though it’s possible for children and adolescents to develop bipolar disorder, it’s a rare occurrence. This makes ADHD the likelier diagnosis compared to bipolar disorder. Another reason to proceed with ADHD treatment is that stimulant medication tends to work quickly. If the symptoms subside after taking stimulant medication, then ADHD is the likely diagnosis. But if symptoms persist, then it’s possible that bipolar disorder is what’s causing them.
If you or a loved one need proper treatment for ADHD or Bipolar Disorder, contact URP Behavioral Health for professional help and support. Here you will receive proper care and advice from experienced and caring specialists.
Co-Occurring Bipolar Disorder and ADHD
How Common is Comorbid Bipolar Disorder and ADHD?
People with a diagnosis of ADHD are eleven times more likely to receive a diagnosis of bipolar disorder. The likelihood of developing bipolar disorder is 30 times greater for those who have a diagnosis of ADHD and anxiety. Research also indicates that up to 1 in 6 people with bipolar disorder have comorbid ADHD.
Due to the similarities between symptoms, people with comorbid ADHD and bipolar disorder may only receive a diagnosis for one of the conditions, which can affect treatment outcomes. Therefore, appropriate diagnosis and treatment are essential for positive outcomes and long-term management of symptoms.
Telling The Difference Between a Manic Episode and Hyperactivity
You can experience a manic episode when you have bipolar disorder, but it’s not indicative of ADHD. Similarly, people with a diagnosis of ADHD may show manic-like symptoms during bursts of hyperactivity. This can also include symptoms like being unable to focus on the task at hand or fidgeting in your seat. The difference, is that the burst of energy associated with ADHD is consistent and may briefly disappear because of external circumstances.
These bursts of hyperactivity associated with ADHD are different from manic episodes, where you feel a decreased need for sleep and an inflated sense of self-confidence. This can last for weeks but eventually results in a depressive episode. The transition from mania to a depressive episode can happen independently, without any influence from external circumstances. So, while there are some triggers that can cause periods of low hyperactivity in ADHD, there’s no need for a triggering event to cause the shift from a manic to a depressive episode.
Diagnosing Comorbid Bipolar Disorder and ADHD
At URP Behavioral Health, we specialize in diagnosing comorbid Bipolar Disorder and ADHD. Our comprehensive evaluations and personalized approaches ensure accurate diagnosis and effective, integrated treatment plans.
Getting a diagnosis of ADHD or bipolar disorder can take time. And if you present with symptoms of both conditions, it can take even longer to get an accurate diagnosis. Due to the overlapping symptoms and similarities between the disorders, your mental health practitioner will need to perform an extensive evaluation.
This can include checking your medical history to see if you have any other health conditions that could be causing symptoms. A treatment facility may also conduct a physical exam and blood tests to determine if your symptoms are the result of substance use. After they’ve ruled out the possibility of your symptoms being the result of a medical condition, they’ll perform a psychological assessment and see if you meet the diagnostic criteria for both conditions.
Diagnosing Bipolar Disorder and ADHD
To be diagnosed with Bipolar Disorder and ADHD, a comprehensive evaluation by a mental health professional is essential. Here’s how each diagnosis is typically approached:
Diagnosis of Bipolar Disorder:
- Clinical Interview: A detailed interview is conducted to gather information about your symptoms, medical history, and family history of mental health conditions.
- Symptom Assessment: The clinician assesses for symptoms of mania/hypomania (elevated mood, increased energy, reduced need for sleep) and depression (persistent sadness, low energy, loss of interest).
- Diagnostic Criteria: The Diagnostic and Statistical Manual of Mental Disorders (DSM-5) criteria are used to confirm the presence of Bipolar Disorder.
- Physical Exam: A physical exam and possibly lab tests are performed to rule out other medical conditions that might mimic bipolar symptoms.
- Mood Charting: Tracking mood changes over time can help in identifying patterns that align with Bipolar Disorder.
Diagnosis of ADHD:
- Clinical Interview: Similar to Bipolar Disorder, a comprehensive interview is conducted to collect information about your symptoms, medical history, and any relevant family history.
- Symptom Assessment: The clinician evaluates for symptoms of inattention (difficulty focusing, forgetfulness), hyperactivity (restlessness, excessive talking), and impulsivity (acting without thinking, interrupting others).
- Diagnostic Criteria: The DSM-5 criteria for ADHD are used to determine the presence of the disorder.
- Behavioral Questionnaires: Standardized questionnaires or rating scales completed by the individual, parents, or teachers (for children) provide additional information about symptoms across different settings.
- Observations: Direct observations of behavior in different settings (home, school, work) may be necessary to confirm the diagnosis.
- Rule Out Other Conditions: The clinician ensures that symptoms are not better explained by another condition, such as learning disabilities, anxiety, or mood disorders.
Combined Diagnosis:
When diagnosing both conditions, it’s crucial for the mental health professional to differentiate overlapping symptoms and understand how each disorder manifests. Accurate diagnosis often requires multiple visits, input from various sources (e.g., family, teachers), and continuous monitoring of symptoms over time.
Treating ADHD With Bipolar Disorder: Therapy in URP Behavioral Health
At URP Behavioral Health treatment center, we treat ADHD with Bipolar Disorder through tailored therapy.
The other component of an effective treatment plan for bipolar disorder or ADHD is almost always therapy. Studies show that therapy is as effective as medication for the treatment of certain disorders. It also helps with long-term recovery by reducing the likelihood of a relapse.
Individual Psychotherapy
This form of psychotherapy involves meeting one-on-one with a licensed mental health clinician to discuss your concerns. For ADHD, psychotherapy can potentially have a greater effect on symptoms than medication alone. You’ll work with your therapist to build study, attention, and emotion skills that improve.
A major benefit of seeking individual psychotherapy is that your clinician can provide tailored support based on your current struggles. In bipolar disorder treatment, therapy serves an important function in changing how you view a situation. Consequently, you’re able to change how you respond to a situation.
Family Therapy
Another mode of therapy that’s often employed to address the symptoms of ADHD and bipolar disorder is family therapy. In the case of bipolar disorder, family-focused therapy is an evidence-based intervention. It comprises three modules, namely psychoeducation, communication enhancement, and problem-solving.
In psychoeducation, the clinician informs your family members about the symptoms of bipolar disorder. As part of this module, your clinician will also teach them coping skills for whenever you experience symptoms, as well as develop a relapse prevention plan. In communication enhancement training, you work on maladaptive communication patterns to practice healthy patterns of interactions. The problem-solving skills module involves building skills to address issues causing conflict at home.
Similarly, family therapy for ADHD helps strengthen relationships by giving your family insights into your symptoms. It also gives them the space to build skills, allowing them to provide the support they need.
Group Therapy
Group therapy sessions increase exposure to activities that reduce ADHD behaviors and increase social skills. In the long term, this can help improve your self-esteem and problem-solving skills as you learn to manage symptoms and achieve your goals. The same applies when you struggle with bipolar disorder since you learn how to solve problems and get a supportive environment to practice your coping skills.
Why Is Treatment at URP Behavioral Health Right for You?
Choosing treatment for ADHD and Bipolar Disorder at URP Behavioral Health is ideal due to our comprehensive and individualized approach. We offer a variety of tailored programs, including individual therapy, group therapy, family therapy, and holistic therapeutic methods, ensuring personalized care for each patient. Our facility boasts exceptional amenities, such as comfortable living spaces, tranquil indoor retreats, secure outdoor areas, and recreational facilities like a basketball court, supporting both physical health and personal growth. Safety is our top priority, with advanced security systems and strict safety protocols in place. Our compassionate, trained staff are always available to provide support and supervision. Our holistic approach, combined with exceptional amenities and expert medical care, ensures a balanced and fulfilling recovery journey. Contact us today to discover how we can support your path to well-being.
FAQs
Here are some commonly asked questions regarding bipolar disorder and ADHD.
Having a diagnosis of ADHD can increase the risk of early-onset bipolar disorder and a higher frequency of mood episodes. If you have ADHD, it will not turn into bipolar disorder, but you may develop comorbid ADHD and bipolar disorder.
The primary differentiator between ADHD and bipolar disorder is time. The hyperactivity associated with ADHD is constant, while the manic symptoms of bipolar disorder are episodic, so they last for weeks before a depressive episode begins. In ADHD, your mood is affected by your environment and external factors, while manic and depressive episodes in bipolar disorder don’t occur as a result of external triggers.
Yes, it’s possible to have co-occurring ADHD and bipolar disorder. The rate of comorbidity between both conditions is high: around 1 out of 13 people with ADHD have comorbid bipolar disorder, while 1 in 6 people with bipolar disorder have ADHD as well.
Let us guide you towards healing
We know that seeking treatment can be overwhelming, but our staff is here to make the process as smooth as possible. We’re available 24/7 to address any questions or concerns you may have.